Psoriasis is an inflammatory, chronic, non-infectious skin lesion with a negative impact on patients' quality of life ("Psora" from the Greek - scales). It is from there, like so many other diseases, that the first observations about psoriasis are described. This term was introduced by Galen, one of the leading researchers in medicine.
The skin signs of psoriasis created confusion between people and doctors, as leprosy was widespread at the time, with dire consequences. Psoriasis patients were subjected to social pressure, were avoided, were isolated by force. In Europe, these people were forced to warn others of their arrival by ringing bells. Treatment attempts consisted of using manure, onions, sea salt, oil, urine, but all were ineffective and excluded psoriasis patients.
PREVALENCE OF PSORIASIS
The disease can occur at any age, but it occurs most frequently in the age group of 49 to 69 years. The reported prevalence of psoriasis in countries varies between 0. 09% and 11. 4%, making psoriasis a serious global problem.
Despite the widespread misconception that psoriasis is not as serious as other non-dermatological conditions, psoriasis creates a disease burden that goes far beyond dermatological symptoms. Its psychological effects are similar to cancer, heart disease, diabetes. Psoriasis plaques are often visible, which can negatively affect interpersonal relationships, academic or professional success. It is not surprising that people with psoriasis experience higher rates of depression with more suicidal thoughts.
Psoriasis patients are also at risk of developing severe comorbidities that complicate disease control and increase the risk of early death. Cardiovascular disease and metabolic syndrome are more common in patients with psoriasis.
In addition, psoriasis is itself a risk factor for cardiovascular disease, tripling the relative risk of developing myocardial infarction. Severe psoriasis is also associated with an increased risk of mortality, resulting in a 3, 5 and 4, 4 year reduction in life expectancy for men and women, respectively, compared to people without psoriasis.
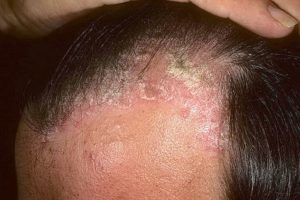
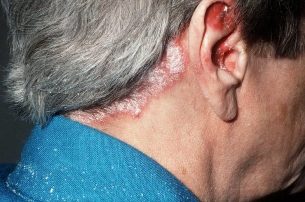
CAUSE OF PSORIASIS IN THE HEAD
There are many theories about the origin of psoriasis. This is the influence of microbes, viruses, allergies, poor hygiene, disturbed blood supply to the skin, disturbance of the functional balance of Organs internal organs, and one of the most urgent ones at the moment is the autoimmune nature of the disease, when the immune cells human beings attack their own tissues. And even that assumption remains a theory, since so far no antibodies that damage the skin have been found in patients with psoriasis.
At the moment, the cause of the pathology remains unknown. But in the course of the research, scientists have identified factors that, with a certain degree of probability, can cause psoriasis.
The following points are highlighted:
- Heredity. There is no one hundred percent chance that, even if the mother and father are sick, their child will necessarily suffer from psoriasis. But, in such a situation, the risk of contracting this pathology is greater. It has also been observed that if an identical twin is ill, the second twin is more likely to become ill than compared to the normal population risk. This proves that this nosology has a genetic background.
- Skin injuries: accidental knife cuts, cat scratches, mosquito bites, sunburn increase the risk of triggering another outbreak.
- Infections: staphylococcal, streptococcal and other infections can also act as triggers. Children often have streptococcal tonsillitis before skin psoriasis begins.
- There are drugs that can trigger the disease, for example, antimalarial drugs, some antidepressant drugs.
- Changing your HIV status to positive can also boost the development of psoriasis. Therefore, testing for HIV when psoriasis is suspected is not strange.
- Stress. The most famous trigger for laymen. "It's all because of stress" - every psoriasis patient has heard this phrase at least once. Some people doubt this phrase, but it has its own justification. Scientists believe that our immune system can respond to emotional and mental pressures, as well as physical defects, such as trauma and infections.
- Excess weight negatively affects the entire body and, if an obese person has a history of psoriasis, treatment is more difficult and generally less effective.
- Smoking. It has been observed for a long time and it is no secret that cigarettes have a negative effect on the condition of the skin. Hence the likelihood of causing psoriasis, especially the damaged head and hands.
- Alcohol is one of the common individual triggers for psoriasis.
- Hormonal changes. The disease usually manifests itself during puberty. Menopause can also cause psoriasis, but during pregnancy there is a decrease or even complete regression of plaques.
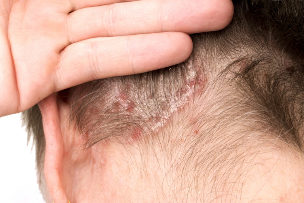
SYMPTOMS OF PSORIASIS IN THE HEAD
In 50% of cases, psoriasis is felt in the head. Psoriasis can appear anywhere on the head. Sometimes small plaques develop that are easy to hide in the hair, but when the entire scalp is covered, it is difficult to hide the plaques.
The appearance of psoriasis on the head will manifest itself as follows:

- Reddish spots on the scalp. Some spots may be barely visible due to fading, but there are also bright red elements that are easy to see.
- Scales that peel off psoriatic skin. The condition of the scalp in this pathology may resemble common dandruff. But there are differences, so, for example, in psoriasis, a silvery glow is observed, and it can also be accompanied by itchy skin.
- Dry scalp. The scalp can be so dry that the skin will crack and bleed, which will create conditions for the worsening of an infection, whose treatment in such a place presents certain difficulties.
- Itching. This is one of the most common symptoms. Someone feels a mild itch, which the patient may forget in daily activities, and some experience an itch so strong that it is impossible to work, study and even sleep.
- Bleeding. As scalp psoriasis can cause itching, the patient can scratch the skin, causing injury. In addition to bleeding, scratching can worsen the course of psoriasis, making the plaque larger and more dense. That's why dermatologists tell their patients, "Try not to hurt your scalp. "
- Recording. The patient can describe his scalp as literally "on fire".
- Hair loss. Rubbing the scalp hard to remove the scales can cause hair loss. Although this phenomenon is temporary, it can still cause inconvenience to the patient.
These clinical manifestations can increase or decrease rapidly. This is an individual process. In one patient, the entire pathological process will end in a pale plaque under the hair, while the other will have many bright spots all over the head. This is influenced, among other things, by the triggers described above.
Several problems that the patient may face:
- Skin manifestations visible to others. Living with psoriasis can make you shy. Any aspect of social life can be stressful for these people, like holding hands on a date.
- Finance. Treatment of psoriasis can be expensive. This is especially true for disseminated psoriasis resistant to conventional therapy, for which new drugs based on monoclonal antibodies are used.
- Pain. Chronic pain can occur with psoriasis, which further increases stress levels. This is especially true when skin manifestations are combined with inflammation of the joints, reducing a person's daily activity.
- Healing. Especially when the patient seeks help late, some procedures do not have the expected effect, which, of course, worries the patient, oppressing him emotionally. Other procedures can take a long time. For example, you may need to receive phototherapy 3 times a week for up to a year. For some, this regime will be difficult to be compatible with the standard pace of life.
- Living with a chronic illness. Psoriasis, like many other chronic conditions, requires great volitional efforts. It is difficult for the patient, especially in the early stages, to deal with a series of additional problems that "fell on his head". This creates conditions for the occurrence of depression.
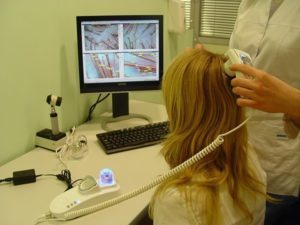
DIAGNOSIS OF PSORIASIS IN THE HEAD
The decision of whether or not to consult a doctor is up to the patient, depending on the severity of the symptoms. However, the best solution, regardless of the location of the plaques, would be to consult a doctor. For further treatment to be as successful as possible, it is necessary to make an accurate diagnosis, even if the symptoms are mild.
In most cases, scalp psoriasis is diagnosed after a physical examination and analysis of the medical history.
A dermatologist is able to determine scalp psoriasis by examining pathological elements of the skin.In exceptional cases, the patient may be advised to have a skin biopsy to rule out other illnesses.
TREATMENT OF PSORIASIS IN THE HEAD
Unfortunately, there is currently no cure for this disease. Therapy is necessary throughout life and aims to maintain remission. In addition, caring for psoriasis patients requires not only skin treatment, but it is also very important to control existing chronic diseases and prevent new ones.
These conditions include cardiovascular disease, metabolic disease and psychological health.
Treatment goals:
- Get the patient's clinical recovery as soon as possible;
- Remission must be stable and long-term;
- Maintain a positive psychological state of the patient.
FOOD DIET
Treatment traditionally begins with diet. Foods containing antioxidants such as vitamin C, E, beta-carotene (vegetables, fruits, sage, ginger and others) can play a positive role, as can omega-3 fatty acids, which are rich in salmon, sardines and other fish.
The link between alcohol and psoriasis is unclear, but experts say that drinkers respond less to treatment and remissions from psoriasis are more prolonged after quitting drinking. In addition, some antipsoriatic drugs are not compatible with alcohol.
A clearer correlation is observed with excess weight. In obese people, as a rule, the pathology progresses more quickly with a brighter clinical picture.
SHAMPOO
Hair makes the treatment of scalp psoriasis particularly difficult. Few people agree to remove their hair to more effectively resolve the clinical manifestations of the disease, especially considering that the defects will be even more noticeable to others.
Conventional hair products are not suitable in this situation, as they can additionally irritate the scalp, contributing to the progression of the pathology. Therefore, tar shampoos are used, whose effectiveness in combating scalp psoriasis has been observed for a long time.
Tar has a "calming" effect on the scalp epidermis, inhibiting the formation of scales. In addition, shampoos with phenolic acid are used, as it has a keratolytic effect (destroys dense corneal scales). Plus is used to increase the penetration of other drugs, including corticosteroids.
When prescribing shampoo, a person's individual characteristics are taken into account in hair hygiene. For example, some women do not wash their hair every day, so it would be best for them to apply the solution to their hair before going to bed 2 to 3 times a week, followed by washing their hair in the morning.
PHENOLIC ACID
Phenolic acid can also be used alone as an ointment. The fact that the ointment is applied for a relatively long time increases its effectiveness of hyperkeratic properties. And for patients who complain about the difficulty of separating the scales from the hair, applying an ointment before the bath can help to solve this situation.

COAL STEP
Coal tar has been used as a treatment for psoriasis for several decades due to its antiproliferative, anti-inflammatory and powerful antipruritic effects.
Although crude coal tar is the most effective resin. Applying raw stone tar to the scalp is problematic. It is generally recommended to use a resin solution (5-20%) formulated as a lotion or added to a corticosteroid. This remedy helps to fight psoriasis, but it has a series of side effects: coloring, hair loss and a more serious negative effect - carcinogenic, for which the use of this method is limited.
For example, for this reason, coal tar is banned in Canada and the European Union.
CORTICOSTEROIDS
Of all the topical treatments available, corticosteroids have been shown to be the most effective in clinical studies for scalp psoriasis and are the most commonly prescribed treatments. Corticosteroids are also convenient because there are a large number of ways of production for any situation: creams, lotions, ointments, oils, gels, foams, solutions, sprays and shampoos.
Do not underestimate the importance of psychological harmony in this pathology. Stress can either become a trigger, causing a detailed clinical picture, or delay the treatment process. Therefore, patients with internal anxiety are advised to consult a psychotherapist, psychologist.
CARE RECOMMENDATIONS FOR HEAD PSORIASIS
It is important for a psoriasis patient to follow the doctor's advice first, but even so, following the simple rules that will be described below, you can further improve the quality of life:
- Use moisturizing lotions. The cutaneous manifestations of the disease are noticeably worse when the skin is dry, so it is important to keep it moist. Specialized cosmetic ointments, lotions or, for example, common petroleum jelly can help with this.
- Take good care of your skin with psoriatic plaques. When washing your hair, never strongly peel off the scales that are adhered to the skin, as you can only spread the process to nearby healthy tissues.
- Be careful when trimming your nails. Cases have been described in which accidental damage to the nail's growth zone with manicure scissors caused the appearance of new skin elements.
- Find the right shampoo for you, that does not peel off your skin, to use on your scalp during remission. Or just continue to use tar, with just less concentration, for daily care.
- The climate can also play a role. It is noticed that the cold negatively affects patients, causing the development of plaques. Sunny weather causes regression of skin manifestations, but not always.
- Use a humidifier. This can keep the skin moist and eliminate dry air, which is bad for psoriasis patients.
- Do not take medications that can harm your skin. The doctor must be informed of any medications you are taking, even those that you consider harmless. For example, for the treatment of depressive conditions, preparations containing lithium salts can be used, which are contraindicated for patients with psoriasis.
- Avoid all types of skin damage: scratches, cuts, bumps. Skin lesions can cause a disease called the Koebner phenomenon (when psoriatic elements develop along the line of damage to the skin). Be careful when shaving. Try to avoid acupuncture, avoid getting tattoos on your body and do what you can to prevent insect bites.
- Try to appear in the sun, but in moderation. The ultraviolet rays of sunlight slow the growth of skin cells, so it is good to receive moderate doses of UV (30 minutes at a time is enough). Excessive exposure to the sun, paradoxically, can cause psoriasis. Also, remember that certain medications can make your skin more sensitive to ultraviolet rays.
- Psoriasis patients should reduce their anxiety level. Of course, it is easier said than done, but relaxation techniques, like meditation or yoga, can be tried.
- Estimate how much alcohol you drink. The link between alcohol and psoriasis is unclear, but scientists still believe it can make symptoms worse, especially in men. It is well known that alcohol is dangerous when combined with certain medications for psoriasis.
- Balance your diet and try to lose weight. If it is difficult for you to do this alone, seek help from experts who can assess in which direction it is worth working better.

RECOMMENDATIONS FOR THE CONTROL OF PSORIASIS OUTBREAKS IN THE HEAD
By monitoring the progression of psoriasis, you can help the patient to better control his illness and take the necessary measures in a timely manner, in addition to increasing the productivity of the doctor-patient relationship. A few simple rules will help you with this:
- Create a “self-portrait” of a psoriasis outbreak. A digital camera, smartphone or just a piece of paper will help you with this, where you can record all changes that occur with the cards. It is also worth noting where the changes initially appear and in what sequence they increase. For this introspection, the doctor will only praise you and know that you are determined. Over time, analyzing the recordings, one can identify standardized situations, for example, an outbreak always begins with a plaque in the occiput.
- Whenever psoriasis regresses or progresses, try to find out what it is. Perhaps the weather has changed? Without medicine? Are you taking a new medication? Recently damaged skin? These triggers can be individual, which makes it difficult for the doctor to understand without the patient's introspection (for example,
 an attack causes a certain type of coffee).
an attack causes a certain type of coffee).
Although the disease is not transmitted by contact, the appearance of patients scares those who do not know. Beauty salons are afraid to provide services, some taxi drivers do not want to transport these people, it is difficult to get a job. Not to mention starting a family, and the fear that their children are condemned to the same suffering prevents them from having children.
There are even cases described where people with psoriasis were unable to train in the Olympic swimming reserve in response to collective complaints from other athletes. Management had to refuse these people, despite the fact that they fully understand that this pathology is not dangerous in the infectious sense.
It is difficult for them to engage in daily activities, since the burden of psychological pressure is high and the person needs social contact. For these reasons, protection and support societies for patients with psoriasis are being formed in many countries. Companies are being sent to educate outsiders about this disease.
People should be judged by their actions, deeds, and not by their appearance. In fact, among patients with such nosology there are doctors, police, firefighters, athletes and many other highly professional people, whose actions not only their relatives, but also their country can be proud of.























