Psoriasis is a disease in which the skin appear red, flaky and scaly lesions covered with silvery-white scales.
Usually these rashes appear on the elbows, knees, the skin of the scalp and lower back but can occur in any other places. Most people have rashes small. In some cases they can itch or hurt.
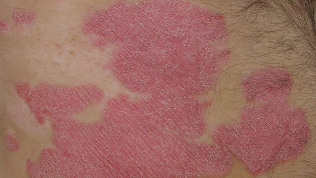
In Russia psoriasis is sick about 1% of the population, often psoriasis is common among indigenous inhabitants of the North. Men and women suffer equally often. First symptoms of psoriasis often appear before the age of 30 years, but a later onset of psoriasis is not uncommon. The severity of psoriasis each person is very different. Someone psoriasis is just a bit annoying, while other people psoriasis prevents lead a normal lifestyle.
Psoriasis is a chronic disease that usually has periods of remission without symptoms or with mild symptoms, after which come the periods of exacerbation, when symptoms become more pronounced.
Psoriasis occurs when the acceleration of the process of reproduction of body cells of the skin. Skin cells are normally made and replaced every 3-4 months, but in psoriasis this process is shortened to 3-7 days. The result is a buildup of skin cells that leads to characteristic changes in the body.
Causes of psoriasis are not fully understood, it is believed that the increased reproduction of skin cells is associated with impaired immune system. The immune system is the natural defense of the body against infections and diseases, but in people with psoriasis it mistakenly attacks healthy skin cells.
Psoriasis can be inherited, and therefore it is considered that this disease is genetic factor. However, it is still unclear what role genetics plays in causing psoriasis.
For many people the symptoms of psoriasis appear or worsen after a specific event, called a trigger. Possible triggers of psoriasis include skin injuries, infectious diseases of the throat and intake of certain medications. This disease is not contagious and cannot be passed from one person to another.
If you suspect psoriasis you should consult a doctor. Often the doctor can make a diagnosis according to the appearance of your skin. Usually for the diagnosis and treatment of psoriasis a patient's guide to a dermatologist — specialist in skin diseases.
Although cure psoriasis is not possible, there are several treatment methods that can alleviate its symptoms and improve the skin's appearance. In most cases, will be primarily assigned to local treatment, for example, vitamin D analogs or corticosteroids local action. In the most severe cases, when not helping out other treatment methods, can be used systemic treatment. Systemic treatment is the ingestion or injection of drugs which have a therapeutic effect on the entire body.
For some people psoriasis is just a small problem, but sometimes it can greatly affect your life. For example, some people with psoriasis have low self-esteem because of how the disease affects their appearance. Often when psoriasis is soreness, pain and swelling of the joints and connective tissues. This is called psoriatic arthritis.
The symptoms of psoriasis
In most cases, psoriasis runs in cycles: every few weeks or months disease exacerbated, and then the symptoms become less noticeable or disappear, and there comes remission.
There are several different types of psoriasis. Many people suffer only one form of psoriasis, although it is possible the disease two different types at the same time. One type can transform into another type or escalate. If you suspect psoriasis you should consult a doctor.
Common types of psoriasis
The usual psoriasis. This is the most common form of psoriasis, which accounts for about 90% of all cases. Symptoms of dry red skin lesions, called plaques covered with silvery-white scales. They usually appear on the elbows, knees, the skin of the scalp and lower back but can appear in any other places. Plaques can itch and (or) hurt. In severe cases, the skin at joints may crack and bleed.
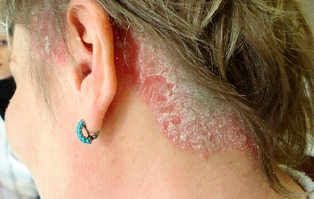
Psoriasis of the scalp (seborrheic psoriasis) may occur on the scalp or on the adjacent skin, as well as on the back and chest. Causing a reddish rash, covered with thick silvery-white scales. Some people have this type of psoriasis causes severe itching, while others do not cause any inconvenience. In the most severe cases can lead to hair loss, often temporary.
The nail psoriasis. About half of patients with psoriasis the disease affects the nails. Psoriasis in your nails can develop small holes or bumps, they may lose color and shape. Often, the nails may eventually become loose and move away from the nail bed, which contains. In severe cases, the nail can crumble.
Psoriasis in the form of droplets are small (less than 1 cm) plaques in the form of drops on the chest, hands, feet and under the hair. High likelihood that the guttate psoriasis completely go away after a few weeks, but in some people it turns into the standard psoriasis. This type of psoriasis sometimes occurs after a streptococcal infection of the throat, and they are more common in children and adolescents.
Folds psoriasis - affects the skin folds such as under the armpits, groin, between the buttocks or under the Breasts. May appear larger smooth rash in some or all of these areas. Symptoms are aggravated by friction and sweating, so we can deliver any inconvenience in hot weather.
Pustular psoriasis
Rarer type of psoriasis, which appear on the skin pustules (vesicles with purulent content). Different types of pustular psoriasis are striking different parts of the body.
Pulstole generalized psoriasis (psoriasis background Tsumbush). Pustules occur on the large surface of the skin and develop very quickly. The pus consists of white blood cells and its appearance is not always directly associated with infection. Pustules can be cyclically re-appear every few days or weeks. At the beginning of these cycles psoriasis background Tsumbush can cause fever, chills, weight loss and chronic fatigue.
Palmar-plantar psoriasis. Pustules appear on the palms and soles of the feet. Gradually turn into blisters rounded brown patches with scales, which are then separated from the skin. Blisters can appear again every few days or weeks.
Pustular acrodermatitis (acrobustulosis). Pustules appear on your fingers and toes. Then the pustules burst, after they leave bright red areas that may bleed or be covered with scales. Can lead to painful deformities of the nails.
Erythrodermic psoriasis (psoriatic erythroderma)
Erythrodermic psoriasis is a rare form of psoriasis, which is almost the entire surface of the skin. It causes severe itching or burning sensation. Because erythrodermic psoriasis your body to lose proteins and fluid. This can lead to other complications such as infection, dehydration, heart failure, hypothermia and exhaustion.
Causes of psoriasis
Psoriasis occurs when skin cells divide and are updated faster than usual. Causes of psoriasis are not fully understood. The body produces new cells in the deepest layer of the skin. These cells gradually move up. Coming to the surface, they die. This normal process occurs gradually and imperceptibly. Skin cells are updated every 3-4 weeks.
In people with psoriasis this process only lasts about 3-7 days. As a result, not fully developed cells can quickly accumulate on the surface of the skin, causing the appearance of red, flaky and scaly lesions covered with silvery-white scales. It is believed that patients with psoriasis skin cells to change faster due to the compromised immune system.
The immune system is to protect the body, which helps him to fight infection. One of the main types of cells, which uses the immune system, called T-lymphocytes.
T-cells normally travel around the body, find the infection and fight with them. In people with psoriasis, they mistakenly attack healthy skin cells. This causes the immune system to produce more T-cells and reproduce new skin cells faster than normal.
It is not clear what exactly causes the disorder of the immune system, although it may be that a certain role is played by certain genes and environmental factors.
Psoriasis is inherited. One of three patients with psoriasis has a close relative with the disease. However, it is still unclear what role genetics plays in causing psoriasis. The results of the study indicate that the development of psoriasis can answer many genes. Likely to make a person more susceptible to this disease, they can different combination. However, inherited not the psoriasis, but only a predisposition, that is, the presence of these genes does not mean that you will necessarily develop the disease.
Triggers of psoriasis
For many people the symptoms of psoriasis appear or worsen after a specific event, called a trigger. If you know your triggers, it can help you to avoid aggravation of symptoms. Examples of common triggers:
- damage to the skin, e.g. a cut, scratch, insect bite or sunburn (the so-called phenomenon Kebner);
- the abuse of alcohol;
- Smoking;
- stress;
- hormonal changes, especially in women (e.g., during puberty and menopause);
- some drugs, such as lithium, some antimalarial medicines, anti-inflammatory drugs, including ibuprofen, ACE inhibitors (for treatment ) and beta blockers (for the treatment of congestive heart failure);
- throat infection — in some people, especially in children and young adults after a streptococcal throat infection is developing a form of psoriasis called guttate psoriasis although in most cases after a streptococcal throat infection psoriasis arises;
- other disorders of the immune system such as HIV that cause the appearance or exacerbation of psoriasis.
Psoriasis is not contagious and cannot be passed from one person to another.
Diagnosis of psoriasis
As a rule, for the diagnosis of psoriasis sufficient external inspection of the skin.
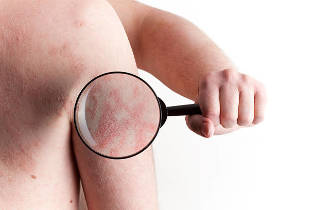
In more rare cases requires a biopsy (small sample of skin), which is then sent to the laboratory for examination under a microscope. This will allow you to identify the specific type of psoriasis and to rule out other skin diseases such as seborrheic dermatitis, lichen planus, simple chronic zoster and pityriasis rosea.
Usually diagnosis and psoriasis treatment is conducted under the supervision of a dermatologist — specialist in skin diseases. If the doctor suspects you have psoriatic arthritis, which sometimes occurs as a complication of psoriasis, you may be referred to a rheumatologist. A rheumatologist is a doctor specializing in arthritis.
You can take blood tests to rule out other diseases such as rheumatoid arthritis and took x-rays of the joints affected by the disease.
The treatment of psoriasis
Completely cure psoriasis is not possible, however, with treatment, could reduce the severity and frequency of exacerbations. Usually psoriasis treatment is under the supervision of a dermatologist, in case of involvement in the process of the joints is assigned to consult a rheumatologist. If the symptoms of psoriasis is significantly pronounced and poorly respond to treatment, your doctor may refer you for admission to the hospital, in the Department of dermatology.
A particular method of treatment is applied depending on the type and severity of psoriasis and the areas of skin affected. If the symptoms of psoriasis are mild and not growing, the doctor may be limited to the appointment of external means, for example, in the form of a cream. In the acute stage typically assigned to the more severe treatment with medications that are taken inside.
There is a wide range of products for the treatment of psoriasis, but it can be difficult to determine which is the most effective means. Talk to your doctor if you feel that the treatment is not helping or you have side effects that cause discomfort.
Treatment methods are divided into 3 categories:
- local treatment to the skin to apply creams and ointments;
- phototherapy — your skin is irradiated with a specific type of ultraviolet rays;
- system — the ingestion or injection of drugs which have a therapeutic effect on the entire body.
Often different treatment methods are combined. As patients with psoriasis requires long-term treatment, it makes sense to have a written plan medicinal manipulations that need to be done daily. The doctor should regularly monitor your condition and, if necessary, to adjust the treatment plan.























